Optimizing Bone Health for Longevity (Part 1)
Bone Health and Longevity Require A Personalized Approach
Loss of skeletal integrity, along with falls and fractures, are some of the well-known and feared consequences of aging. After a hip fracture, there can be loss of mobility, and restricted function, and there is a significantly increased risk of mortality within one year. My intent in this two-part blog is to dispel some of the myths around causes and corrections and to deepen your understanding of testing and treatments that can be done. We will discuss how we personalize the approach to maintaining or restoring lost bone. We will not be reviewing the basic prevalence and epidemiology of osteoporosis, as those facts are found elsewhere in detail. Click on this link for one such resource.
Aging and Bone Remodeling: The Composite Structure of Bone
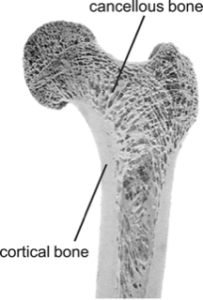
The fibrous “matrix” is the foundation of bone structure, made of a specific collagen protein (mostly type 1 collagen) wound in triplicate, to which minerals are bound, called “hydroxyapatite”. This mineral matrix is what gives the collagen its rigidity and density. Bones have an outer shell, called the cortex, which is thick and resists bending, but remains light. The center of bone, where the bone marrow is located, has a different, more fragile bony lattice called the trabecular bone (sometimes called cancellous bone). This distinction will be important in a few paragraphs when we talk about measuring the trabecular density, which is rarely done, but possible. The trabecular bone needs to be dense and intact to maintain the outer shell, the cortex. Over our lives, we are in a constant state of micro-injuries and aging, happening side by side with constant repair, and the whole process of breaking down and repairing is called bone remodeling.
Bone Loss With Aging: Are Calcium and Vitamin D Enough?
We reach our peak bone mass around age 30 and we are in decline in our 40s, and in women, we are losing bone density even BEFORE estrogen levels start to decline. Despite the common advice to take vitamin D and calcium, deficiency of those two substances is rarely the key cause of osteoporosis, and supplying those two nutrients has not consistently produced a significant chance of improving osteoporosis once it is present.
A recent Cochrane meta-analysis of 7 randomized controlled studies (2023, referenced below) did not find overall a significant beneficial effect of calcium and D supplementation for improving bone mineral density. Individual studies in the past have sometimes found beneficial effects, for example, the updated Osteoporosis Society meta-analysis study in 2016 showed a 15% overall decreased risk of fracture with calcium and vitamin D supplementation. However other positive studies showed very minimal benefits, and there are many negative studies as well. Whether calcium and D actually work is still considered somewhat controversial due to differing interpretations of three different large analyses.
This is not to argue one shouldn’t be taking them, just to point out that if calcium and vitamin D worked well, we would not have needed over 34 drugs studied and approved to treat osteoporosis. It would be a simple preventable condition, which it isn’t. If calcium and D do work, it is a marginal effect, not a cure. We want to focus on the triggers and mediators of bone loss that aren’t discussed at a typical primary care or endocrine visit and to encourage you to think about your own physiology and the factors that may be contributing, as well as how to address them.
Factors in Bone Loss: Nutrition and GI Health
There are many nutrients we need to keep up with our active busy lives, and even more nutrient support may be needed if we are more athletic, are fighting some type of chronic inflammation, or have gastrointestinal or microbiome imbalances. Some signs that you might be suffering from nutrient insufficiencies are nail abnormalities (white spots, flattening, ridges, pitting, inflammation around the nail bed), hair that is dry, brittle, thin or lifeless, skin, if bumps are on the back of the arms, dry and scaly scalp, seborrhea, eczema, cracking at the edges of the lips, decreased taste or smell, yellow or white or inflamed tongue, cavities or premature tooth loss or periodontal disease, muscle spasms or weakness. These are all potentially indicative of a need for more nutritional or supplemental support.
A second source of bone loss can be from an unhealthy GI tract. If you have bloating, belching, multiple food sensitivities, constipation or diarrhea regularly, abnormal stools or undigested food in stool, pale or floating stools, you may have a chronic digestive impairment that can contribute to ongoing bone loss. We want to correct digestive and nutrient imbalances from the root cause, even if we choose to start with medication as a first therapy. You should find an experienced provider to chase down and test properly for these various issues and not self-diagnose from Dr. Google or ChatGPT!
Longevity Medicine Considers Many Factors When Evaluating Bone Loss
Here are some factors, a partial list, that we consider in an evaluation for an adult in mid to late life with bone concerns:
- Magnesium intake and levels (Red blood cell levels may be more accurate than serum)
- Vitamin D levels- some of us have Vitamin D receptors that don’t bind as well, so the bare minimum level is probably not the best target)
- Morning urine pH (optimal > 6.5.)
- Intake of alkalizing minerals (magnesium, potassium, sodium, calcium, and trace minerals too)
- Gluten sensitivity- if present
- Homocysteine levels (potential inflammatory issue if higher than optimal)
- Protein intake (age over 60 the recommended protein targets are higher)
- Vitamin K intake
- Inflammation (generally, in the body)
- Estrogen levels- optimally at least 20-30 estradiol (by LCMS, not MS, testing in older women)
- Strength training program- evaluating if sufficient or if overtraining
- Growth Hormone levels
- Microbiome health (digestive health)
How Can I Improve My Bone Health? To Medicate or Not to Medicate
As you can see from the above partial list, we at Hudson Valley Longevity Medicine are doing a much more holistic and comprehensive look at factors that will help maintain bone health through the aging process. These factors are important to consider, EVEN IF you do choose to go on medication as medications may not work as well without an optimization of these factors. In addition, many medications are only prescribed for a limited amount of time and some people don’t tolerate medication.
Some patients may be able to reverse their bone loss without medications if they understand the factors that are important for them. As you can see, telling a patient with osteopenia to walk more and take calcium and vitamin D is not a comprehensive or fair answer to “How can I improve my bone health?”
What is DEXA Testing? Why is It Important to Bone Health?
Most of us are familiar with the very safe and rapid DEXA test which gives you a score (related to overall density) for your lumbar spine, hips, and sometimes wrists. Some radiology centers can provide another parameter, called the “trabecular bone density” or “TBS” if they have the proper software. This newer parameter is very useful to an interested healthcare provider as a decision support tool because it deepens our sense of urgency or comfort with respect to fracture risk. It also provides a benchmark for follow-up to make sure our therapies are improving the INTERNAL part of the bone, not just the cortical thickness.
Ask your radiology center if they have this software and if not, look for a center that can do this. In the past, a CT scan has been used to evaluate the inside structure, but this is done mainly for research and involves significant radiation. There is a blood test called “C-telopeptide” or “CTX” that you can get at most commercial labs, that gives you a sense of ongoing resorption (loss), with higher levels indicating more ongoing bone loss. Again, this data can act as a decision support tool, deepen your understanding of what is going on in your body, and act as a benchmark that can be followed later to adjust therapies.
Your Healthy Aging Plan Should Include Bone Health
We know that bone health is a complicated area, but as you can see, it’s also an important piece of our healthy aging plan that has the potential to be addressed through lifestyle factors, dietary change, exercise prescription, gut repair, and supplementation. We highly recommend the book, The Whole-Body Approach to Osteoporosis by Dr. McCormick referenced below, which is detailed and will start you on your own evaluation, but you will need a careful and knowledgeable guide to deploy complete testing and a comprehensive lifestyle plan. In our next blog, we will review some less well-known methods and guides for change, and highlight some of the newer tools that are available to be combined with medication or on their own, to maintain our skeletal structure and ensure our ability to move around and function well into our later decades.
Contact us if you have questions or request an appointment If you’re interested in working with us as a longevity medicine patient at Hudson Valley Longevity Medicine.
Resources
The Whole-Body Approach to Osteoporosis: How to Improve Bone Strength and Reduce Your Fracture Risk book by R Keith McCormick, DC
Management of osteoporosis in postmenopausal women: the 2021 position statement of The North American Menopause Society – Very good overview of incidence, assessment, and general treatment strategies (pharmacologic)
Calcium and vitamin D for increasing bone mineral density in premenopausal women – Recent Cochrane review of calcium and vitamin D studies, although note other meta-analyses reached different conclusions
Photo by RDNE Stock project



